Lumbar Laminectomy
What is a Lumbar Laminectomy?
A lumbar laminectomy involves removal of the bone and ligaments that are causing compression of the spinal nerves in the lower back (spinal stenosis). Typically, when these nerves are being compressed, it is due to a combination of enlargement of the facet joints, thickening of the ligamentum flavum and bulging of the intervertebral discs. The classical symptoms are what is termed “neurogenic claudication” where there is pain on walking in the calves or buttocks. Usually back pain is not a feature, and the pain is related to standing or walking and relieved with rest. Sitting or lying improves the pain. Bending forward, such as with a shopping trolley also improves the pain. Occasionally the pain is almost entirely in one leg and typically this is due to lateral recess stenosis, where the nerves on one side are compressed more than the other side. If spinal stenosis is not treated, it may progress or it may stay the same. Rarely, it will improve. Like most degenerative conditions, it is not fatal and the patient is unlikely to end up in a wheelchair if not operated upon. Surgery is usually aimed at improving pain.
Anatomy
If we look at the typical anatomy of the region shown in the anatomy section, and then at the figures below, the features of spinal stenosis become clear.
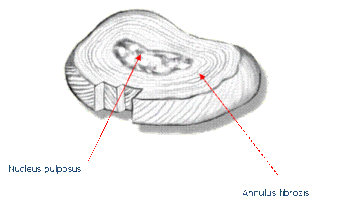
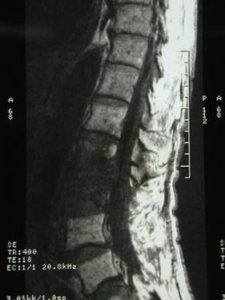
Preop MRI scan showing spinal stenosis secondary to facet joint arthrosis and ligamentous hypertrophy at the L45 level.
Immediate postoperative CT scan showing the extent of bone and ligament removal.
Reason For Operation
The indication for surgery is failure of conservative management for neurogenic claudication. It must be stressed that surgery is an option, not a necessity, once spinal stenosis is diagnosed. Typically a laminectomy is performed and the neural foramina, through which the nerves exit, are enlarged (foraminotomy).
Technique
The procedure is quite straightforward and involves the removal of the spinous processes, laminae and ligamentum flavum with a combination of biting instruments of various size and configuration, and sometimes small high speed drills. At the end of the decompression, the neural foramina are palpated to ensure the nerves move out easily. A multilevel laminectomy can lead to moderate blood loss and occasionally a blood transfusion is required. Typically, however, this is not the case.
Risks
The risks of the operation relate to specific risks from this kind of surgery, and general risks which are independent of the type of operation performed. General risks include the risks of death, heart or lung problems, pneumonia, bleeding, infection, clots etc. etc. Typically this is <5-10%. The specific risks include the risks of nerve injury, spinal fluid leakage, instability (increased ‘floppiness’ which may cause problems later on and require further surgery) etc. etc. would also be at approximately 5-10%. The risk of death or ending up in a wheelchair is however low, but both can and have happened.
Expectations
The likelihood of a good outcome is always tailored to the individual patient, but in a typical scenario, the chances of good or excellent improvement in symptoms, including possibly complete resolution of preop symptoms is 80-90%. No one can guarantee a 100% risk-free operation and no surgeon can perform an operation with no risk. Most patients do well from this surgery. This is not a good operation for back pain.
Recovery
Surgery typically takes 1-2 hours and in an uncomplicated case the patient is mobilized the next day. A tube may be placed in the bladder and this is usually removed once the patient is mobilized. After surgery, the patient is usually mobilized the the same night or following day, and all things going well is discharged from hospital 1-3 days after surgery. The back is sore where the incision is but this settles. Dissolving sutures are usually placed in the wound. Once home, it is important to avoid bending, lifting, twisting and prolonged sitting for four weeks postop. You should see your family doctor one week after surgery for an inspection of the wound. You need to look after the wound to ensure good healing. Typically I advise my patients not to rub any creams on the incision and to keep it dry. Bathing is to be avoided, as is swimming but showering is OK. It is important that the wound is allowed to heal. Any signs of redness, discharge, swelling, etc. needs to be reviewed by a medical practitioner. Follow-up with the specialist is usually arranged for six weeks after surgery.
Non-Surgical Options
Unfortunately no good non-surgical options are available. Walking is certainly helpful and advisable and physiotherapy and hydrotherapy can help any associated back pain. Weight loss may also help and avoidance of bending, lifting and twisting is important as well. All the previous measures may help but in dealing with a structural lesion it is understandable why failure of conservative treatment can occur. Because spinal stenosis is not a life-threatening condition, the decision to have surgery is entirely up to the patient; if the patient can live with the pain then surgery can be avoided.
Other Points
Lumbar laminectomy is a common operation and is performed regularly in patients over the age of 65. Age itself is not a contraindication. Although no guarantees can be made, most patients do well, with no complications. The results are poorer and the risks higher with redo surgery, and each reoperation has greater risks and a worse outcome than the previous operation.
